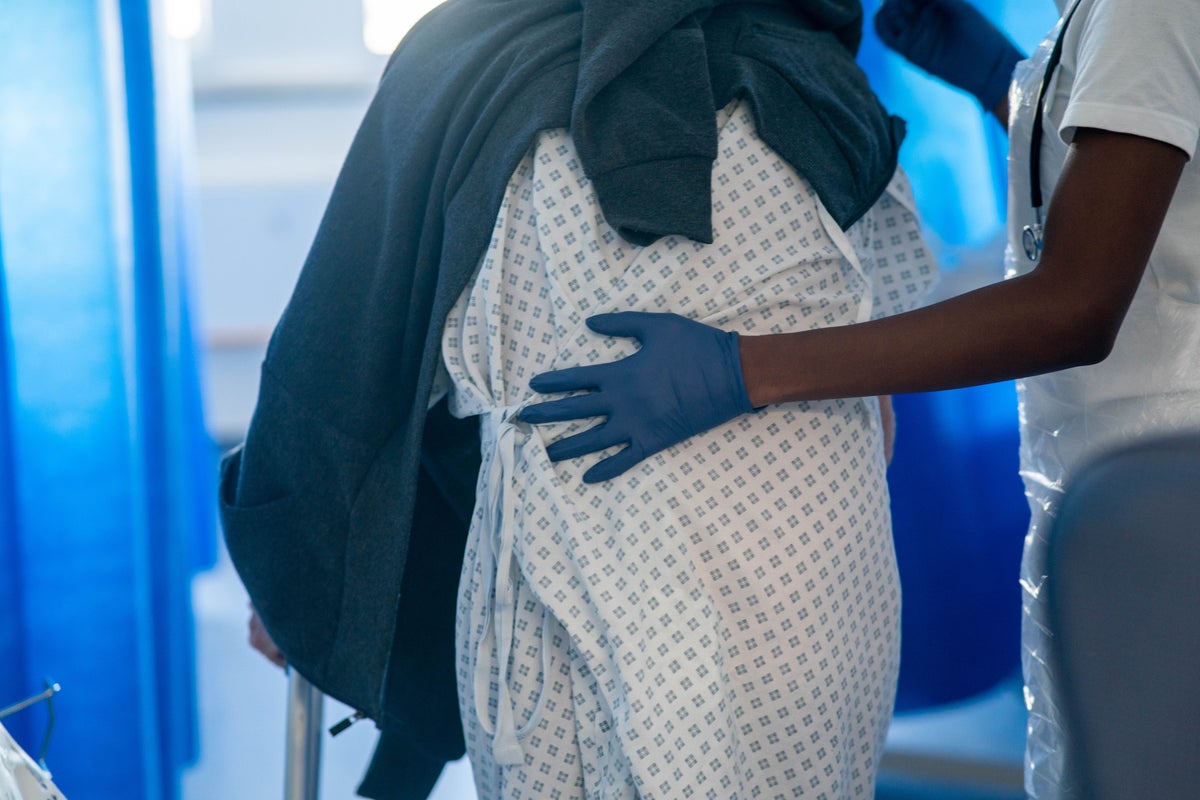
The NHS has become “reliant” on private companies, charities and social enterprises to deliver routine mental health care, a think tank has warned.
New analysis by the King’s Fund found more than one in four NHS mental health inpatient beds is being outsourced.
While the independent sector provides vital surge capacity for the health service during periods of high demand, the think tank said the NHS has moved “far beyond” this, exposing it to the risk of higher costs and longer stays in hospital for patients.
A new report by the King’s Fund said that between January and March 2025, NHS trusts reported almost 18,000 available mental health beds, with 89.5% of these occupied.
However, its analysis shows that in March, an additional 7,195 beds were available in the independent sector for NHS use.
This is around 29% of NHS-funded mental health bed capacity in England, the think tank claims.
Siva Anandaciva, director of policy at The King’s Fund, said: “Independent sector health care capacity acts as an important release valve for many NHS services when they face periods of high demand.
“It would make no sense to leave private beds empty when the NHS could purchase spare capacity and patients still receive care free at the point of use.
“However, our analysis reveals that there has been a significant increase in the share of NHS mental health inpatient care being outsourced to independent providers.
“Far beyond acting as valuable surge capacity, the NHS has become reliant on the independent sector for delivery of routine mental health care.
“This exposes the health service to greater risk of higher costs, could leave patients facing longer stays in hospital, and means the public has less transparent data about the quality of services.”
The research also found the independent sector is providing an increasing proportion of care for patients with the most complex needs, including those with learning disabilities, autism and people with diagnosed personality disorder.
Mr Anandaciva added: “For the NHS to be sustainable in the long term, there needs to be far more focus on providing care in the community that keeps people well.
“Traditionally, the mental health sector has made great progress in delivering community-based care.
“However, some patients with greater or more complex mental health needs may need inpatient care, and the NHS must do all it can to treat people in the appropriate setting for their health needs.”
Responding to the findings, Minesh Patel, associate director of policy and campaigns at mental health charity Mind, said: “Dangerously high bed occupancy rates and an overreliance on the private sector are yet more evidence of the underfunding of NHS mental health services and the mental health estate.
“But sadly these are not the only worrying trends that have become commonplace in mental health services.
“Run-down buildings that people describe as more like prisons than hospitals, people becoming more unwell because they can’t get the help they need in the community, an outdated Mental Health Act that enables coercive and racist treatment – these and many more harmful trends in mental health care have, over years of decline and de-prioritisation, been normalised.
“If the UK government is serious about shifting care from hospitals to the community, and from sickness to prevention, it must engage with the many systemic issues in mental health care that have been allowed to take root.”
An NHS England spokesperson said staff are working hard to manage “record demand” with the roll-out of 24/7 mental health centres and more support in schools.
They added: “We are also supporting health systems to develop plans to ensure mental health patients receive quality care close to home if they require an admission to hospital.
“The NHS has repeatedly made clear that all services must provide safe, high-quality care, irrespective of whether they are NHS or independent sector led, and we continue to work closely with the CQC to monitor, identify and take appropriate action where it is needed.”
